|

Related
References for The Leapfrog Group Hospital Ratings:
Jack Pattie Show, July 8, 2014
Back to Video Presentation
References on Adverse Events:
“Using a weighted average of the 4 studies, a lower
limit of 210,000 deaths per year was associated with preventable harm in
hospitals. Given limitations in the search capability of the Global Trigger
Tool and the incompleteness of medical records on which the Tool depends,
the true number of premature deaths associated with preventable harm to
patients was estimated at more than 400,000 per year. Serious harm seems to
be 10- to 20-fold more common than lethal harm.”
From: James JT. A New, Evidence-based Estimate of Patient Harms Associated
with Hospital Care. Journal of Patient Safety. Sep. 2031 9(3):122-128 PMID:
23860193
http://journals.lww.com/journalpatientsafety/Fulltext/2013/09000/A_New,_
Evidence_based_Estimate_of_Patient_Harms.2.aspx
---------------------------------------------------------
13.5% of hospitalized patients had a serious “adverse
events”
An additional 13.5% of patients had “temporary harm” events.
In addition, “28%” of the 13.5% of patients who had a serious event also had
”temporary harm”
Over all at least 44% of these events were judged as being preventable.
Patients could have multiple events (such as the 28% of the 13.5% of
patients with serious events also had temporary harm events).
From: Levinson, DR. Adverse Events in Hospitals: National incidence among
Medicare beneficiaries. November 2010 OEI-06-09-00090
http://oig.hhs.gov/oei/reports/oei-06-09-00090.pdf
---------------------------------------------------------
Medical Errors may be the third leading cause of
death in the United States
http://www.propublica.org/article/how-many-die-from-medical-mistakes-in-us-hospitals
---------------------------------------------------------
"As many as 65%-70% of cases of CABSI (Catheter
Associated Bloodstream Infections) and CAUTI (Catheter Associated Urinary
Tract Infection) and 55% of cases of VAP (Ventilator Associated Pneumonia)
and SSI (Surgical Site Infections) may be preventable with current
evidence-based strategies. CAUTI may be the most preventable HAI. CABSI has
the highest number of preventable deaths, followed by VAP."
From: Umscheid CA, Mitchell MD, Doshi JA, Agarwal R, Williams K, Brennan PJ.
Estimating the proportion of healthcare-associated infections that are
reasonably preventable and the related mortality and costs. Infect Control
Hosp Epidemiol. 2011 Feb;32(2):101-14.
http://www.ncbi.nlm.nih.gov/pubmed/21460463
References on Problems With Self Reporting:
“The poor state of voluntary facility reporting was
documented in a March 8, 2010 OIG Report which found that in surveyed
hospitals, patient diagnosis codes were inaccurate or absent for 7 of the 11
Medicare Hospital Acquired Conditions identified by physician reviewers and
reviewed hospitals did not generate incident reports for 93% of the
events.(1)”
“An observation included in this report was from officials at the Joint
Commission who estimated that only 0.1% of sentinel (severe) events are
reported.(2) In addition, a July 2016 Joint Commission report stated that
only 9,637 reports of sentinel events from general hospitals had been received since January
1995.(3) Only 64.6% of these reports were identified by self-reporting.(3)
An AHRQ survey found similar results with 48% of 614 facilities (with
143,052 respondents) that did not report any adverse events (sentinel or
otherwise) at their institution.(4) Finally, the AMA News reported that as
of 2007, approximately half of U.S. hospitals had never reported a physician
to the National Practitioner Data Bank that was established in 1986.(5)”
(1) Levinson DR. Adverse Events in Hospitals. Methods for Identifying
Events. March 2010. Office of Inspector General. Dept. of Health and Human
Services. OEI 06 08 00221
http://oig.hhs.gov/oei/reports/oei-06-08-00221.pdf
(2) Levinson DR. Adverse Events in Hospital: Overview of key issues. Dept.
of Health and Human Services, Office of Inspector General. Dec 2008, Page
25, 32
http://oig.hhs.gov/oei/reports/oei-06-07-00470.pdf
(3) Sentinel Event Statistics. The Joint Commission. March 31, 2010.
http://www.jointcommission.org/NR/rdonlyres/377FF7E7-F565-4D61-9FD2-593CA688135B/0/SE_Stats_9_09.pdf
Summary Data of Sentinel Events Reviewed by The Joint Commission. July 5,
2016.
https://www.jointcommission.org/sentinel_event_statistics_quarterly/
(4) Sorras J. Hospital Survey on Patient Safety Culture: 2009 Comparative
Database Report . AHRQ March 2009
http://archive.ahrq.gov/professionals/quality-patient-safety/patientsafetyculture/hospital/2009/hospsurv091.pdf
(5) Sorrel AL. When is conduct reportable? National Practitioner Data Bank
takes complaints from hospitals about physicians. American Medical News Sept
21, 2009
http://www.ama-assn.org/amednews/2009/09/21/prsa0921.htm
From: Financial Incentives to Promote Healthcare Quality: The Hospital
Acquired Conditions Nonpayment Policy. The Journal of Social Work in Public
Health. 2011 Sep 26(5):524-541. PMID: 21902485
http://www.tandfonline.com/doi/abs/10.1080/19371918.2011.533554&
-------------------------------------------------------------------------------------------------------------
A study of three major hospitals found that errors
occurred in one in three patients and that 90% of these errors which not
have been identified by standard tracking systems from the Agency for
Healthcare Research and Quality.
From: Classen DC, Resar R, Griffin F, Federico F, Frankel T, Kimmel N,
Whittington JC, Frankel A, Seger A and James BC. ‘Global Trigger Tool’ Shows
That Adverse Events In Hospitals May Be Ten Times Greater Than Previously
Measured. Health Affairs. April 2011 vol. 30 no. 4 581-589.
http://content.healthaffairs.org/content/30/4/581.abstract/a>
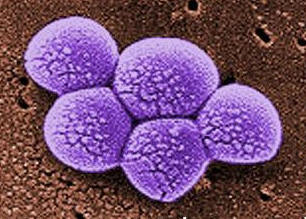
The pictures on the right and left are photomicrographs of
Methicillin-resistant Staphylococcus Aureus (MRSA).
|
